After first hearing about Doximity’s partnership with Saving Mothers in early 2022, I eagerly filled out my application. It was during my trip home from an energizing company offsite in Miami when I learned I was selected to go to the Dominican Republic with Saving Mothers as a Doximity representative. I was excited for the opportunity to support an organization whose mission is crucial to improving the lives of mothers and newborns around the world.
Landing in Santiago and meeting the team
Two weeks later, I landed in the Dominican Republic’s third most populated city, Santiago de los Caballeros. Far from the resorts of Punta Cana or Santo Domingo, Santiago is nestled between two mountains in a valley about 140 km from the Haitian border. The World Bank considers the Dominican Republic an upper-middle-income country. By many indicators, the Dominican Republic is experiencing rapid growth, with an annual GDP growth rate of 12.3% and a life expectancy of 74 years; however, one metric that highlights the need for a group like Saving Mothers is the country’s stubbornly high maternal mortality rate (see graph below). The national estimate of mothers who die per 100,000 live births has hovered around 95 since 2009. The rest of the region is closer to 72 and trending down. Saving Mothers is one piece of the puzzle working to reduce maternal mortality rates.
The day I arrived, I met up with our Saving Mothers team. We had dinner close to our hotel and made a game plan for the week. Dr. Sasha Hernández, an OB/GYN from New York, led our small but mighty team. The team also included Dr. Anjali Dogra, an anesthesiologist from New York, Dr. Leise Knoepp, a urogynecologist from New Orleans, Paxton Voigt, a medical student from New York, and Guillermo Peraza, a senior operations manager from Proximie – a health technology platform that enables surgeons to virtually attend operating rooms to guide complex surgeries visually. Our local champion, Dr. Beralis Ramos, was instrumental in coordinating our access to the local OB/GYN team.
My first day
Our main goals of the week were to evaluate patients for surgery, prepare the postpartum hemorrhage kits for simulation practice, and organize the Saving Mother’s office space. My job as the Doximity representative was to support our team whenever I could. Every day I would organize lunch pickup with our driver and make trips to the back office for supplies. I helped set up the OR for sterile surgeries and occasionally helped with pre or post-op patient care. I took photos and videos of procedures, presentations, and our team with some of the incredible staff at the hospital. Each day we left the hospital tired but motivated.
On Monday morning, our task was to visit four patients who had previously been recommended for consults by our Saving Mothers team. All four patients were recommended for either hysterectomies to treat uterine prolapse or vaginal slings to treat stress urinary incontinence. One surgery was performed on our first afternoon. While Dr. Leise was operating, Guillermo broadcasted the surgery via Proximie’s remote technology to the Saving Mother’s team in New York. The service allows remote visual access to cameras in the OR and on the laparoscopic equipment. He trained doctors in the hospital to set up the connection and fielded questions from the OB/GYNs joining remotely. I delivered lunch for the team and some residents watching the surgery with Guillermo. We wrapped up the day with dinner at the hotel and went to bed early.
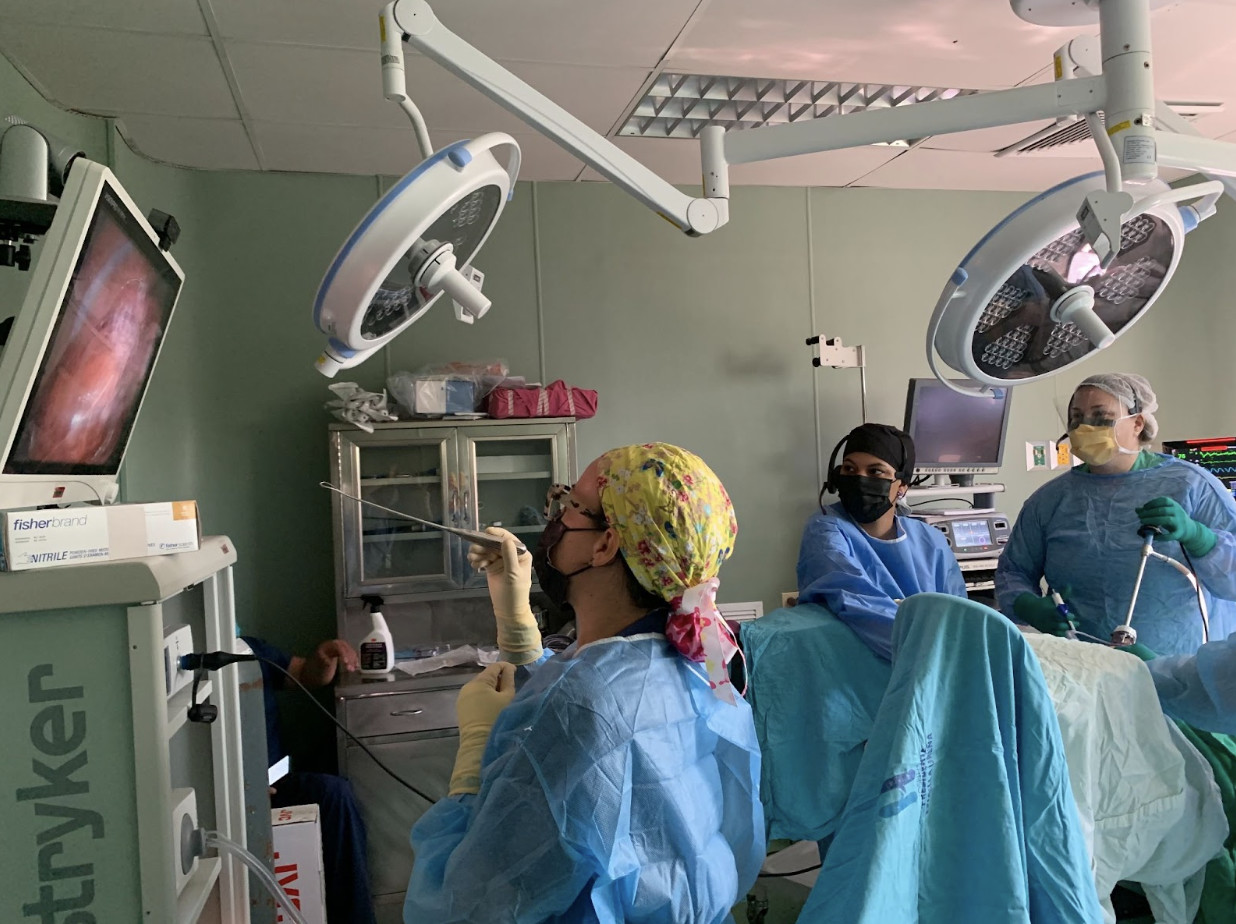
Helping build out postpartum hemorrhage kits
By Wednesday, we were in our routine of early mornings and surgeries. The two surgeons and the anesthesiologist performed a total of four surgeries, two were performed laparoscopically with an emphasis on training the OB/GYN residents on laparoscopic hysterectomy. I’ll never forget seeing a patient's uterus on the scrub table. It was smaller than I expected, about the size of a small fist. All surgeries were successful and the patients recovered well. After the surgeries, our focus shifted to our other main objective, the postpartum hemorrhage kits and simulation.
The value of simulating emergency scenarios cannot be overstated. Practicing before an emergency allows the medical staff to nail down the most efficient procedure to save lives. Studies show that when medical staff have access to checklists and practice emergency procedures, mortality decreases. While the Saving Mother’s doctors were performing surgeries alongside the hospital’s residents, one of my jobs was to help build out the postpartum hemorrhage kits with Paxton (see photo below). The kits contained all the lifesaving tools a medical team would need to stabilize the patient during a hemorrhage.
While one trip will never solve the problems of something as complex as maternal mortality, processes like simulations and kits and checklists can make a profound difference.
While most of the postpartum hemorrhage kit equipment was donated and shipped from the U.S., we had to purchase some things locally. With our driver, Dr. Ramos and I traveled to local pharmacies to collect medication and equipment, like syringes and distilled water for IV bags. It was nice getting out of the hospital and seeing more of the town while accomplishing a helpful task. Once all our equipment was purchased and organized, we started filling the kits and prepping for our simulation that afternoon.
Taking part in emergency simulations
Paxton kicked us off with a presentation on the value of simulations and what the audience would be expected to do. We had a full house of attendings, residents, nurses, pharmacists, pediatricians, and some medical students. Everyone who would play a role in a real postpartum hemorrhage was asked to attend. Paxton then asked for a few volunteers to start the simulations. This was my time to shine. I was asked to play the patient – setup with special pants that would include an infant, a placenta, and a bag of fake blood with a small hose for simulated hemorrhage. Paxton told me to sell it. I screamed and grunted my “baby” out, “birthed” my placenta, then opened the line to let the “blood” flow. Now the simulation had started.
The lead doctor reviewed the checklist and called out what needed to be done. Nurses and residents handed him some supplies from the kit. A resident “administered” the misoprostol, a drug that induces uterine contractions, and simulated the placement of an IV. They worked fast, and I was “saved.” The team and audience then discussed what could have been done better and what went well. They mentioned how the kits would be a great tool because one of their biggest challenges is waiting for all the supplies to arrive from disparate locations. Overall, the simulation was a success.
Ending the trip with more simulations and reflections
On our last day, we did more simulations, this time in the operating room to give it a more realistic setting. Different doctors took turns being the lead doctor, and each nurse got a chance to participate. I nearly lost my voice from “giving birth” so many times, but I didn’t mind laying down on the OR table after a week on my feet! Everyone found it to be a good experience, and there seemed to be healthy discussion comparing and contrasting the simulation to their past postpartum hemorrhage cases.
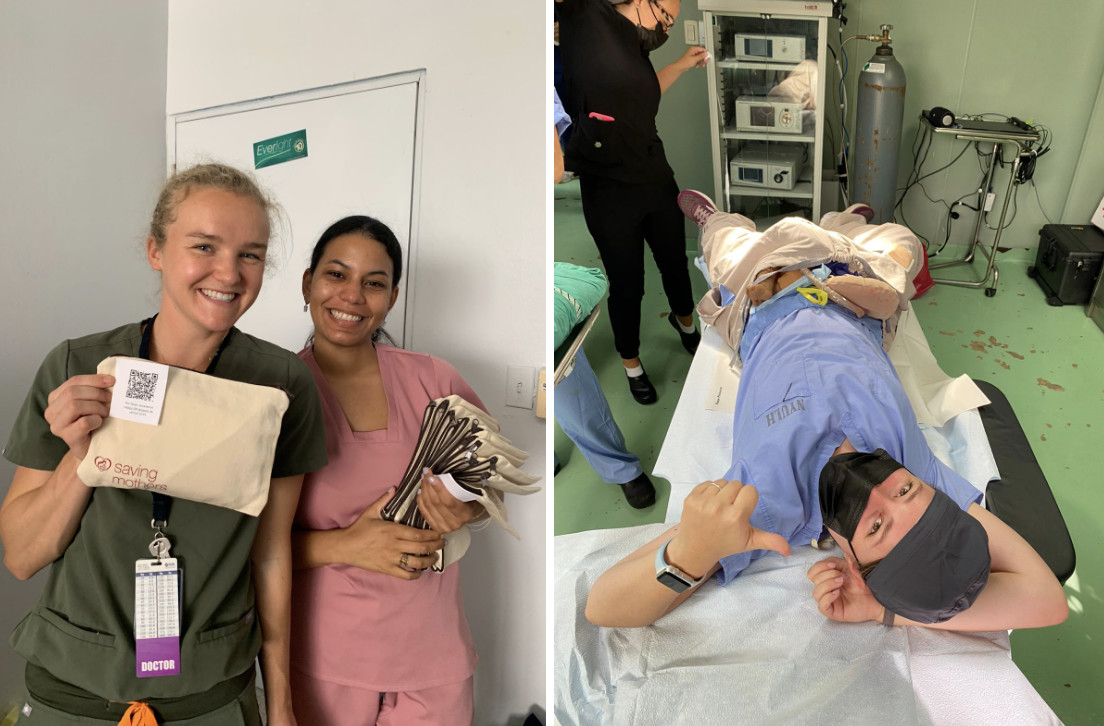
One aspect of the kits I found impressive was the QR code on the kit, which linked to a survey. Paxton asked the staff to take the survey after any future PPH cases. To incentivize participation, she offered a gift card to a randomly selected respondent. This is such a valuable way to get insight into how successful a project is. Surveys are an important tool in capacity-building projects because they identify future improvements.
While one trip will never solve the problems of something as complex as maternal mortality, processes like simulations and kits and checklists can make a profound difference. I’m proud to represent Doximity, a company that supports this work by putting physicians first, and I’m honored to have personally supported a group of healthcare professionals committed to saving lives.

